 
But 2022 saw the first drop in deaths since 2009. The researchers suggested that the decreased deaths rates from Alzheimer's disease, as well as Parkinson's disease, were "perhaps due to early-pandemic increased incidence of each due to misattribution of COVID-19 deaths when there was limited testing and considerable COVID-19-related missed medical care. The pandemic accelerated that trend, making 2021 the deadliest in US history, with more than 3.4 million deaths. Alzheimer's disease: 12.6% and 14.2%, respectively.Influenza/pneumonia: 14.6% and 16.0%, respectively.On the other hand, large decreases in years of life lost and deaths from influenza/pneumonia and Alzheimer's disease were noted:   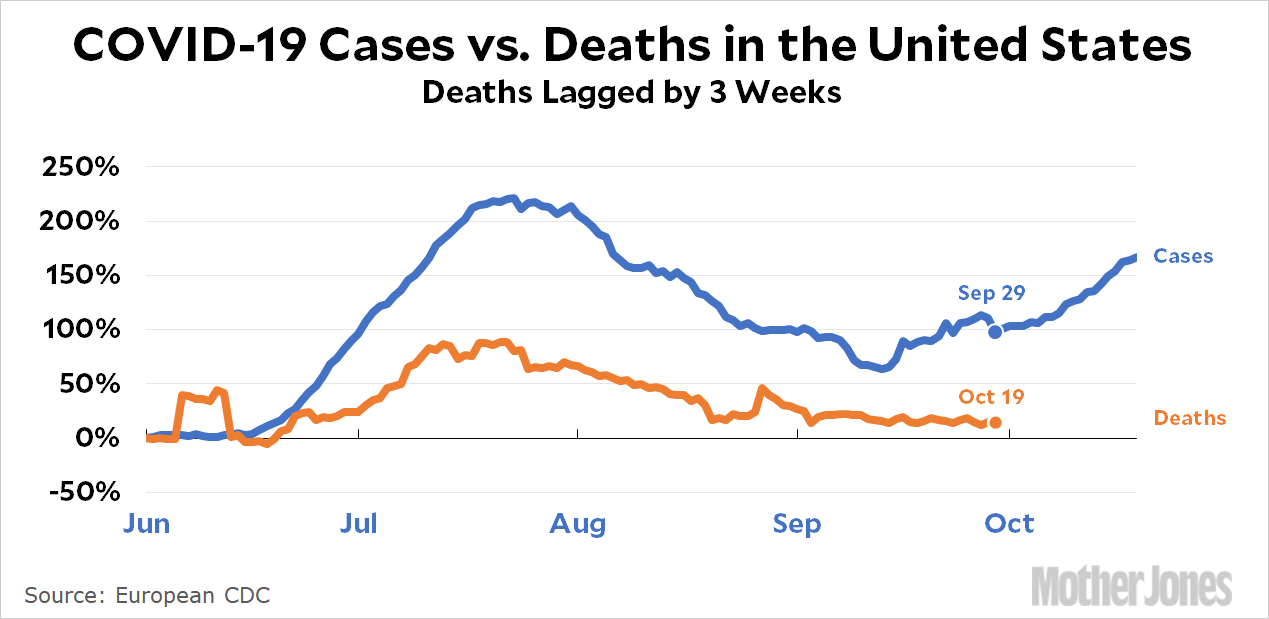
Among three of the four causes of death with greater than 10% changes in death rates during the study intervals, concordant changes were seen in years of life lost.Ĭonsiderable increases in both years of life lost (10.5%) and deaths (11%) due to unintentional injuries were observed, which the researchers suggested was partially due to the "record-high drug overdose deaths" that increased by 15% in 2021 - resulting in nearly 14,000 deaths - versus 2020. However, there has been a rise in death rates among younger individuals and a decline among older individuals in 2021 versus 2020, "reflecting excess premature mortality from COVID-19," the authors noted.Īcross both study intervals, years of life lost linked to most of the leading causes of death were stable. Previous reports have indicated that similar COVID-related death rates occurred from March to December 2020 and from January to October 2021. Over 1 million COVID-related deaths occurred from March 2020 to September 2022 in the U.S. "Understanding this shift in COVID-19 mortality dynamics could inform prevention and treatment approaches, public policy development, and community measures to minimize future effects of COVID-19," they added. "Further investigation should determine the extent to which this downward age shift in COVID-19 mortality is attributable to high early-pandemic COVID-19 death rates among older adults (for example, involving nursing homes and long-term care facilities), relatively higher vaccine coverage and adherence with nonpharmaceutical interventions among older versus younger adults later in the pandemic, age-related risk differences associated with coronavirus variant viruses, or other mechanisms," the researchers wrote. I think it's quite possible that we're having right now, as many cases as we were during the, you know, the delta wave of August or September, certainly not what we had this past winter, but we probably are having a lot more cases than what's currently being reported.Overall, years of life lost per COVID death increased by 35.7%, while years of life lost due to any other cause of death did not change by more than 2.2%, they noted in a research letter published in Annals of Internal Medicine. "I would not be surprised to find out that our confirmed case count is under-counting the total number of cases by a factor of two or three. "We're probably missing a lot," David Dowdy, an epidemiologist at the Johns Hopkins Bloomberg School of Public Health, told ABC News last week. The "high" community-level transmission suggests there is a "high potential for health care system strain" and a "high level of severe disease." Thus, the Centers for Disease Control and Prevention recommends people wear a mask in public indoor settings, including schools.Īs infection rates continue to increase across the country, some health experts are questioning how much higher totals are than initially reported. MORE: Indoor masking recommended again in Northeast counties 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
